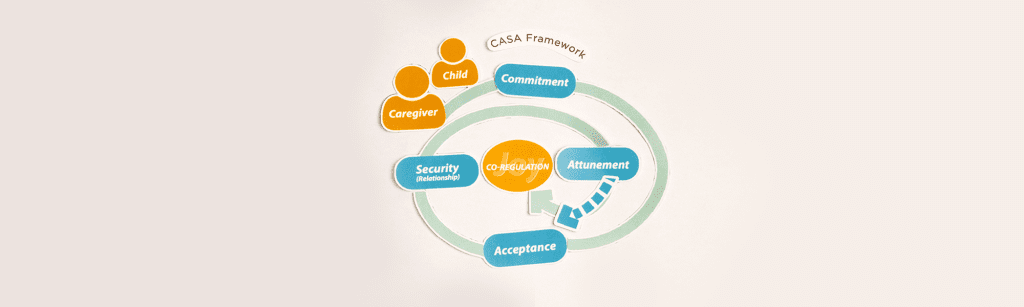
Supportive Treatment Programs for Youths
We offer a wide network of programs providing various levels of mental health treatment for male, female, and LGBTQ+ adolescents, teens, and young adult youths aged 12-28.
Mental Health Treatment Centers for Teens and Young Adults
With mental health treatment centers nationwide, Embark ensures its comprehensive care is easily available to all adolescents, teenagers, young adults, and their families.
Flexible Insurance Solutions
Recognizing the importance of mental health care for your family, we offer flexible payment and insurance options.

Aetna

Allegiance

Anthem

Blue Cross Blue Shield

Care First

Carelon

Cigna

Health Link

Kaiser

Providence

United

Valley Health Plan
Overcome Mental Health and Substance Use Challenges
We’re here to help your adolescent, teen, or young adult heal mental health issues such as:

A Transformative Treatment Approach

Start Healing
Contact Us
Begin the path to healing by filling out our simple online form, our admissions counselors will walk you through the healing journey.
Take an Assessment
Take the next step in the healing journey by taking a mental health assessment to understand your child's unique needs and challenges.
Start Treatment
After the assessment and personalized plan, your child starts their journey to healing and joy at the location that best meets their needs.